Combating stigma and discrimination to promote the treatment of TB patients
- Posted on 07/11/2023 14:08
- Film
- By abelozih@sante-education.tg
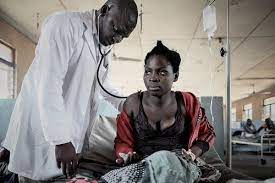
Extract from the article: The Knowledge, Attitudes, Practices and Beliefs (KAPB) survey carried out in Togo in 2012 on tuberculosis confirmed that powerful metaphors associating tuberculosis with death, guilt and punishment, crime, horror and "others" built and legitimised th
The
Knowledge, Attitudes, Practices and Beliefs (KAPB) survey carried out in Togo
in 2012 on tuberculosis confirmed that powerful metaphors associating
tuberculosis with death, guilt and punishment, crime, horror and
"others" built and legitimised the stigma established at the start of
the epidemic. The use of this language can be explained by another aspect that
underpins and reinforces the stigmatisation process: people are afraid of fatal
diseases. This is the case of the Ewe language, spoken mainly in Togo,
"YOME KPE", which literally means "the cough of
death". The stigma is partly based
on people's fear of the consequences of TB infection, particularly the high
case-fatality rates (especially when treatment is not widely available), the
fear of transmission or of seeing someone with advanced TB decline rapidly.
In
Togo, rejection, stigmatisation, discrimination and marginalisation of people
with tuberculosis are still a reality. And yet, like many other diseases,
tuberculosis can be treated and even cured free of charge.
At
what levels of society is discrimination associated with tuberculosis?
At
several levels: First of all, in the family or community context, what is
sometimes described as "effective" stigmatisation: these are acts
which push individuals to do things, or forget to do things, which put others
in danger or deny them services or rights. Examples of this form of
discrimination against people with tuberculosis include: ostracism; shunning
the person or avoiding contact with them on a daily basis; verbal harassment;
physical violence; discrediting and verbal reproaches; gossip. Secondly, in the
institutional environment, particularly in the workplace, healthcare services,
prisons, educational establishments and social centres. This discrimination
translates actual stigmatisation into institutional policies and practices that
discriminate against people with TB, or on the contrary, into the absence of
anti-discrimination policies or redress procedures. Examples of this form of
discrimination against people with TB include: health care services,
workplaces, schools and learning centres, prisons, families.
At national level, discrimination may reflect stigmatisation that has been officially sanctioned or legitimised by laws and policies that have already been put in place and promulgated in the form of practices and procedures. This can further reinforce the stigmatisation of people with TB and therefore legitimise discrimination.In many countries, laws have been enacted to restrict the rights of people and groups affected by TB.These include compulsory screening and testing of groups and individuals; prohibition of recruitment of cured TB patients for certain positions and types of employment; compulsory isolation, detention and medical examination and treatment of infected persons; restrictions on foreign travel and migration, including TB testing for persons applying for work permits abroad, and deportation of foreigners with TB.Discrimination can occur by omission, for example when laws, policies and procedures to redress and safeguard the rights of people with cured TB are not applied or are lacking.
Who
are the most stigmatised people when it comes to tuberculosis?
Tuberculosis is more common among people facing social and economic inequalities, particularly those living in poverty and overcrowded conditions (prison environments) and people living with HIV.
What
are the possible consequences of stigma and discrimination?
The
consequences of the stigma associated with tuberculosis for patients and
communities can be: Social: for example, isolation and loss of opportunities
for family support.By blaming particular individuals or groups who are
'different', others may avoid recognising their own risk, confronting the
problem and taking care of those affected. Portrayals of people with TB in the
media and on television that suggest it is a 'disease of poverty', a 'disease
of infidelity', a 'superstitious disease' or a misinterpretation of the link
with HIV can reinforce stigma. This last idea is reinforced by the concept of
sin in religious belief, which also supports and reinforces the idea that HIV
infection is a punishment for deviant behaviour.
There are economic consequences: for example, the loss of a job or paid leave, or refusal to be taken back on after recovering from tuberculosis. There are also medical consequences: many patients who appear to be carriers of the germ on the basis of the few symptoms detected reject the disease and do not go to the clinic so as not to become suspects, also, for example, unfavourable health outcomes, including death, and an obstacle to the recruitment of health workers in the community). Stigma and discrimination therefore prevent people from getting tested, recognising that they are ill, and seeking care and psychosocial support. The lack of any significant reduction in the incidence of tuberculosis over the past decade reflects our inability to tackle its underlying social causes, including stigma and discrimination against people with the disease.
Is
the NTP faced with this scourge of stigmatisation and discrimination of people
with the disease?
The
June 2012 national survey on knowledge, attitudes and practices relating to
tuberculosis in Togo reveals that patients "complain of being isolated,
marginalised or arousing feelings of mistrust.A minority choose voluntary
isolation. Stigmatising patients and
refusing to sleep with them are negative reactions. In all regions, and more
particularly in Lomé Commune and the Maritime region, the proportion of people
who say they refuse to sleep with a tuberculosis patient is low. Attitudes such as abandoning the patient or
indifference represent very low proportions overall. This represents a major advance in people's
attitudes to tuberculosis. But this progress must be maintained.
These
representations can lead to a defeatist attitude towards illness, mistrust and
rejection of the patient. On the one hand, believing that the disease
inevitably kills is an attitude that does not encourage dynamic action to
combat it.It will be essential to use communication messages to try to reverse
this negative attitude. On the other hand, there is a lack of knowledge or
awareness of the disease.The public needs to be properly informed, with a clear
distinction drawn between the real causes and the risky behaviour that
encourages contagion. Clearly, if two smokers exchange cigarette butts, for
example, or two lovers kiss and breathe together when one of them has
tuberculosis, the risk of contagion is very high, and in some cases
unavoidable.However, tobacco, alcohol and adultery are in no way factors that
cause tuberculosis.
What
has been done to combat the stigmatisation of TB patients?
At
a global level, the Dahdaleh Institute for Global Health Research at York
University in Toronto has spent the last 15 years studying and addressing the
healthcare drivers of TB, in particular the stigma of TB and its impact on
treatment adherence among people with drug-resistant disease and HIV
co-morbidity.Much of her research is based in South Africa, where she draws on
the perspectives of patients, providers and the community to help develop
person-centred approaches to TB and TB-HIV care.
In
Togo, awareness campaigns are also aimed at providers and the
community.Providers must be ethical and deontological so as not to divulge
information about a patient to anyone.The community is made aware of these
issues through discussion forums and other means. The patient's community is a source of
healing. The work of associations and NGOs helps to raise awareness of
illnesses and health in general. Key messages: « You can eat with a TB
patient who is taking his medication without being contaminated » « After
two weeks of taking medication correctly, the risk of contamination by the
patient decreases. » « We need to give our TB patients moral and
material support, so that they can quickly regain their health. » « When
a patient is on anti-tuberculosis treatment, they must not miss any medical
appointments. Their lives and the lives of others depend on it. »
Pour
les patients qui sont des fonctionnaires ou des salariés, ils ont le droit
d’être protégé par leur hiérarchie et d’être soutenu. Après guérison, ils
doivent regagner leur poste. On ne doit pas les licenciés ou les pénalisé du
fait qu’ils ont fait la TB. En bref, lutter contre la stigmatisation, un
déterminant social incontrôlé de la tuberculose.
Source
: PNLT




